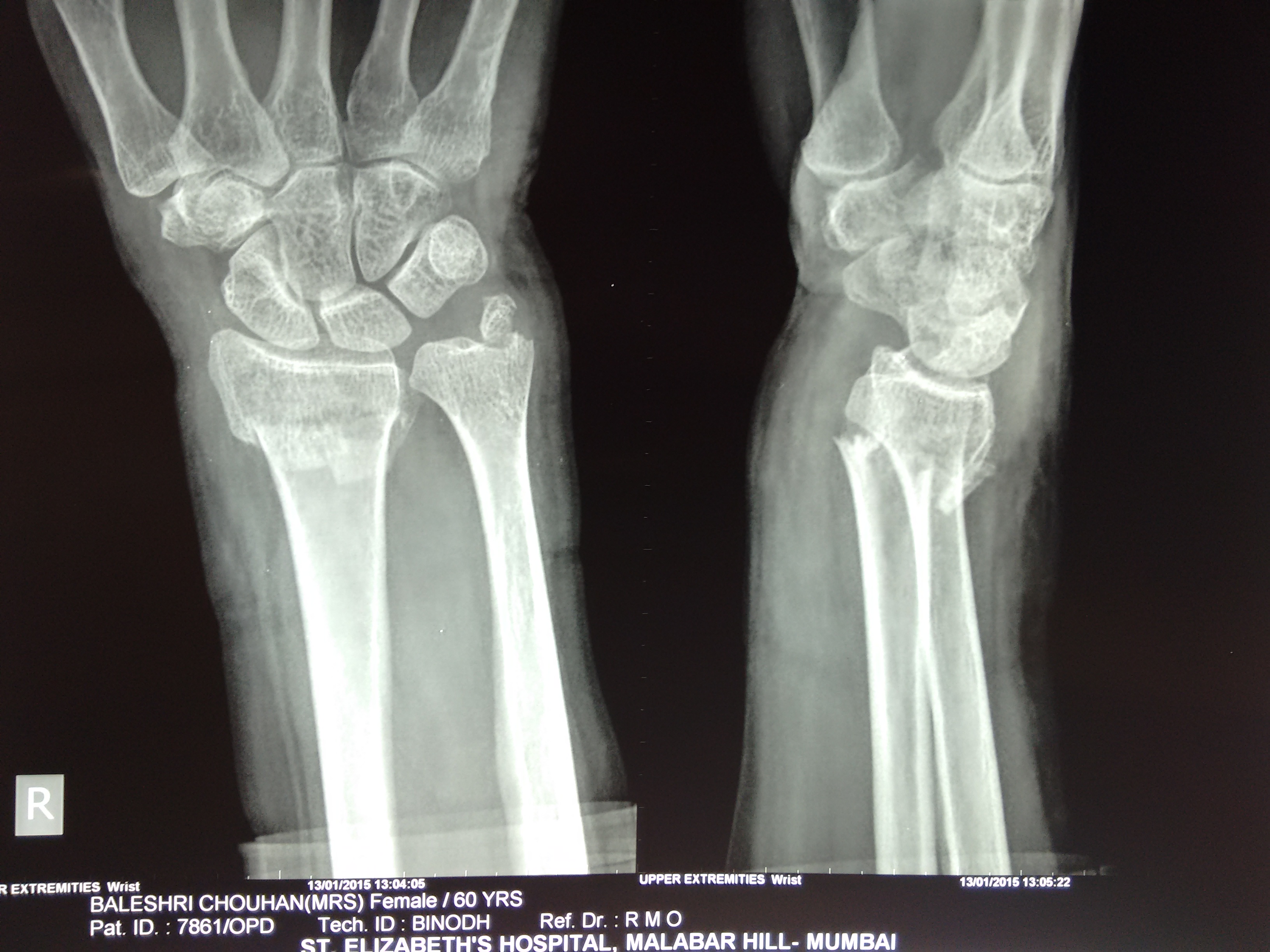
Relevant imaging investigations include: 6 Bone profile if suspecting osteoporosis (vitamin D, serum calcium, ALP).Relevant laboratory investigations include: Blood sugar monitoring (BM): if there is suspicion of a hypoglycaemic episode as a reason for the fall.Urine dipstick: if there is suspicion of a UTI causing confusion as a reason for the fall.Electrocardiogram (ECG): if there is suspicion of cardiac involvement in the fall.The range of motion of the wrist is typically pain-free. Fracture of the radial shaft: less common than distal radius fractures.It typically presents with local tenderness over the ulnar styloid. Ulnar styloid fracture: fracture of the ulnar styloid may be associated with distal radius fractures.However, the main complaint is typically localised pain and tenderness over the anatomical snuffbox (triangular depression over lateral, dorsal hand). Scaphoid fracture: commonly caused by a FOOSH as well.The clinical presentation of fractures of the distal radius is similar to several other fractures of the wrist: 5 The sensory distribution in the hand of the radial, ulnar and median nerves. Sensory: the tip of the second digit (digital cutaneous branch) and thenar eminence (palmar cutaneous branch)įigure 1.Pulselessness and/or pallor of the hand (suggesting vascular compromise)įor suspected distal radius fractures, the neurological examination should also include assessment of the median, ulnar and radial nerves (Figure 1).Loss of sensation or movement distal to the fracture (suggesting nerve injury).Open wound and/or the bone protruding through the skin (open fractures require different management due to the risk of infection).Less common clinical findings may include: Tenderness on palpation of the distal radius.Pallor: pallor or duskiness of the hand (suggesting vascular injury)Ī thorough orthopaedic examination of the hand and wrist, along with a neurological examination of the upper limb should be performed to assess functional capacity and neurovascular deficits.Pain: disproportionate to the injury (suggesting compartment syndrome).Paraesthesia: tingling, pins and needles or loss of sensation in the hand (suggesting nerve injury).Social history: smoking and alcohol (risk factors for osteoporosis), occupation (may influence the choice of management)įor more information on falls, see the Geeky Medics guide to the assessment, investigation and management of falls.Īlthough less common, it is important to ask about symptoms which may suggest neurovascular injury including the 3P’s:.Family history: a family history of fragility fractures, especially parental hip fractures, is a risk factor for osteoporosis.Past medical history: risk factors for osteoporosis, previous fragility fractures, co-morbidities. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
